|
What
are the causes of overweight in childhood? |
A small
percentage of overweight cases in childhood are
due to hormonal abnormalities, but
the vast majority of childhood overweight is due
to
over-eating.
It is pretty simple:
if children take in more calories than they burn
up, they will gain
weight. Some kids may have
"higher
metabolism
rates" and burn
up food faster, but
even if a child's
metabolism rate is high, if they eat
excessively, they
will gain
weight.
|
Weight problem vs. Eating Problem |
Children who are overweight generally
refer to themselves
as having a
"weight problem", but in actuality what they have is an
"eating
problem." They eat more than they burn up by physical activity.
Lack of activity can contribute
to overweight.
Kids today are not as active as in the past. But
over-eating is by
far the biggest
contributor to
gaining
weight. For example, walking several miles is required in order to burn up
just one ice cream cone. The
reasons for
excessive food
intake are not that
complex.
Depression,
anxiousness, low
self-esteem, stress, or just boredom are
commonly relieved by food. We do not feel
pleasure and
emotional pain at
the same time.
Unfortunately, the
emotional pain returns as soon as
the food is
consumed.
| Psychological dependence on food |
Using food as a way
to neutralize emotional pain can
actually result in
a psychological dependence on food.
The child becomes psychologically
"hooked"
on food to keep from feeling emotional discomfort, very similar to a drug
addiction. Resisting overeating to begin with takes "will power", but
breaking psychological food dependence takes heavy duty will power.
Tolerating life's pains, finding alternative comforting things, and distracting
oneself by fun activities is necessary to avoid psychological food dependence.
There is also the
"Vicious Circle
Effect."
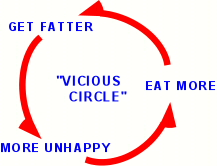 Once a
child
gains excessive
weight, the
decrease in
self-esteem and
social isolation
associated with
being overweight
causes more
depression, anxiety, and stress, so that seeking comfort in food and overeating
increases even more, with more weight gain, worse self-esteem, and so on.
This is referred to as a "vicious circle". And the heavier a child becomes, the less he/she is
able to move around to burn calories, further increasing weight gain, i.e. a
second vicious circle. To lose weight requires breaking these vicious
circles. The child must realize that overeating and gaining more weight will just increase
the
unhappiness and problems with exercise and make it even more difficult to do something about the weight.
Finding other comforting things that don't involve food, distracting fun activities, and support groups can help break the vicious circle. Once a
child
gains excessive
weight, the
decrease in
self-esteem and
social isolation
associated with
being overweight
causes more
depression, anxiety, and stress, so that seeking comfort in food and overeating
increases even more, with more weight gain, worse self-esteem, and so on.
This is referred to as a "vicious circle". And the heavier a child becomes, the less he/she is
able to move around to burn calories, further increasing weight gain, i.e. a
second vicious circle. To lose weight requires breaking these vicious
circles. The child must realize that overeating and gaining more weight will just increase
the
unhappiness and problems with exercise and make it even more difficult to do something about the weight.
Finding other comforting things that don't involve food, distracting fun activities, and support groups can help break the vicious circle.
|
Parental nurturing can help turn off emotional eating. |
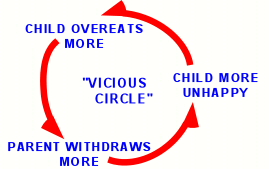 Children who do not receive emotional comfort at home may turn to food for
comfort. A nurturing relationship with parents can turn off the emotional
appetite for food. Unfortunately, overweight in their child tends to upset
parents, so that the relationship becomes strained, which causes the child to
seek more comfort in food, which upsets the parents further, i.e. another
vicious circle. And parents may feel that overweight in their child is the
parents' fault. But it is no one's fault, just misunderstanding.
Breaking the vicious cycle by loving and nurturing your overweight child is the
key. Talk to your child about his/her feelings, what feelings are being
numbed by food, and help the child to learn to
find comfort and stress relief in things other than food. Again, if you
have not read it, please see How Do I Lose Weight? Children who do not receive emotional comfort at home may turn to food for
comfort. A nurturing relationship with parents can turn off the emotional
appetite for food. Unfortunately, overweight in their child tends to upset
parents, so that the relationship becomes strained, which causes the child to
seek more comfort in food, which upsets the parents further, i.e. another
vicious circle. And parents may feel that overweight in their child is the
parents' fault. But it is no one's fault, just misunderstanding.
Breaking the vicious cycle by loving and nurturing your overweight child is the
key. Talk to your child about his/her feelings, what feelings are being
numbed by food, and help the child to learn to
find comfort and stress relief in things other than food. Again, if you
have not read it, please see How Do I Lose Weight?
| A
craving is
different than
hunger. |
Hunger is what we
feel when our body
is lacking in the
nutrition of
food. A craving
is what we feel when
we want the pleasure
of food. If
your child eats for
pleasure rather than
for nutrition,
excessive weight
gain is usually the
result. Help
your child to learn
how to eat for
nutrition rather
than for pleasure.
|
Practice
portion
control. |
The size of food
portions in our
culture is set by
people who want to
sell food.
Eating the
"standard
size" portions
in most restaurants
on a regular basis
will cause most
people to gain
weight. One of
the best ways to
control your
children's weight is
to let them eat
whatever they like,
just less of
it. To help
them lose weight, it helps to
cut whatever they
normally eat by half or a
third and save the remainder for later. Once
the weight loss has
occurred, to
maintain it, the portions are then made just a
small amount less
than they used to
eat. Portions can be adjusted to keep your child's weight in the healthy range.
| Being
overweight can harm your child's health. |
The problem with obesity in children and teens is not just the cosmetic and
self-esteem issue of looking
"fat". Obesity can seriously harm your child's health. If
there is excessive fat on the outside of the body, there is also excessive fat on the
inside, i.e. in the body's organs. Fat build up in organs such as the
heart, the arteries, the liver and pancreas causes these organs to function
poorly.
Diabetes (Type 2) is on an alarming rise in
the adolescent population. Type 2 diabetes is intimately
related to being overweight. Type 2 diabetes was rare in kids 20
years ago, but the rate of type 2 diabetes in kids has increased by one percent
every year since 1980, in parallel with the increase in obesity in kids13.
High blood pressure is also increasing at an alarming rate in children.
Similar to type 2 diabetes, high blood pressure in children is likewise related
to being overweight. And if a teenager has high blood pressure and is
overweight, they have a 90% chance of having high blood pressure as an adult, with a high risk of an artery breaking in the brain (stroke).14.
Overweight children have more bone and joint problems,
 simply because of the
mechanical stress which the extra weight puts on bone and joint structures. simply because of the
mechanical stress which the extra weight puts on bone and joint structures.
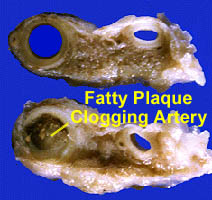
The high fat, high sugar foods
which overweight kids and teens eat cause
fatty deposits called "plaque" (pronounced "plack") to form on the inside of
the arteries supplying organs like the heart, the brain, and the kidneys. This
plaque, shown in the lower artery on the left, eventually blocks normal flow of blood to those
organs (the upper artery is normal). Moreover, pieces
of plaque can suddenly break off and totally block the blood flow
downstream. This results in a "heart attack" in the case of the heart or a
"stroke" in the case of the brain. Plaque deposits also cause
"hardening of the arteries", which results in high blood pressure,
kidney failure, and broken arteries in the brain, another form of stroke.
It is known statistically that the longer the child carries the weight, the greater the risk to the child of becoming an overweight adult.
90% of overweight teenagers becoming overweight adults. Obese adults have a
much higher rates of diabetes, high blood pressure, heart attacks, strokes, and cancer.
| The medical definition of
"Overweight". |
"Medically overweight" is different than "socially
overweight." "Socially overweight" means that a child is embarrassed
about their weight and gets teased about it. The term "medically overweight" means that a child's weight is
a risk to their health. Doctors use what is called the "Body Mass
Index" or BMI to determine if a child is medically overweight. The
BMI is also used for adults and indicates how much fat a person has on their
body.3,4 The BMI changes normally with a child's age.
For example
children less than 3 years old and teenagers have more fat normally on their
bodies than children 4 to 12 years old so their BMI is higher.
The BMI is simply a number that shows how a person's weight
relates to their height, in other words whether their weight is proportionate to
their height. The BMI is the weight divided by height multiplied by
itself. BMI's for children in the typical U.S. population are listed on
the National Center for Health
Statistics website. A thing called the BMI "percentile" is
used to compare how a child's BMI relates to other children their age and
sex. For example, if your child's BMI is at the 75th percentile, that
means that his or her BMI number is greater than seventy-five out of a hundred
kids their age and sex. If a child has a BMI higher than the 85th
percentile they are considered "medically
overweight", and if greater than the 95th percentile then they are
considered "medically obese." How was that percentile
picked? It was determined by a
committee of
experts on obesity in kids.9
Actually it is Mother Nature that determines what a healthy BMI is, because a child's BMI percentile is related to health risks.
Three out of five children and teens with a BMI above the 95th percentile
have at least one risk factor for cardiovascular disease. One out of five
children with with a BMI above the 95th percentile have two or more risk factors
for cardiovascular disease. 5
Overweight children are likely to become overweight adults.
1,6
The extremes in BMI-for-age that raise concern in children 2 to 20 years of age:
BMI-for-age <5th percentile: Medically
underweight
BMI-for-age >85th percentile:
Medically overweight
BMI-for-age >95th percentile: Medically
obese
You can find out your child's BMI percentile and
whether they are medically overweight and at health risk by using the percentile
calculator on our site. This calculator uses the
recently released height, weight, and BMI percentile charts of the U.S. National
Center for Health Statistics.
| How
do you know if your child has a weight problem? |
Ten Ways to Tell if Your Child Has a Weight Problem*
1. His/her doctor tells you so.
2. Your child complains about being teased about her/his size.
3. Your child’s clothes seem to get too small too fast.
4. Shopping for clothes with your child is a nightmare.
5. Your child refuses to be seen in a bathing suit.
6. Your child’s friendships are suddenly changing.
7. Your child withdraws from activities he/she previously enjoyed.
8. You find yourself referring to him/her as "big-boned" or "large."
9. You notice your child huffing and puffing after a simple task such as climbing of stairs.
10. Your child tells you she/he thinks she/he is over-weight.
While excessive weight gain can occur at any age, many parents don’t address the issue until the child is older and it has become a much
bigger
problem. When you wait until it’s a problem of larger proportions, it’s harder to treat.
*From The Can-Do Eating Plan for Overweight Kids and Teens., by
Michelle Daum, MS, RD, a pediatric nutritionist in private practice in Westchester and Long
Island, NY.
| Does your child
need to lose weight? |
Your doctor or healthcare provider is the best source of
information on weight loss in children and teens. For information on
weight loss in children and teens, please click on the following links to the
Healthy Weight
School:
DOES YOUR CHILD NEED TO LOSE WEIGHT?
WHAT IS SAFE WEIGHT LOSS IN CHILDREN AND
TEENS?
A recent poll asked kids on
this site what they thought would reverse the growing overweight problem in
children and teens. Most kids responding felt that the solution is:
"Parents realizing that their kids will have shorter
lives, stopping their own overeating, and being role models for their kids."
|
Tips
to help prevent
children from
overeating:
|
1)
A child's good
eating habits begin
with the adults in
the home.
Children will mimic their
parent's good and
bad eating habits.
And, if only high
fat, sweet
and
low-nutrition food
is mostly available,
this is what the
child will eat.
Parents
need to be role
models for healthy
eating and active
lifestyles.
2) Do not use
food as a reward or to comfort or soothe. Teach your child that food
is what his/her body needs to run on for fuel and to make new parts like bones and
muscle, rather than something for entertainment or to comfort bad feelings.
3)
Help your child to
find sources of comfort,
pleasure, and fun
other than food. Hobbies,
sports, and clubs
can relieve boredom
and offer
distraction from
depression and
anxiousness.
They will also
increase
activity. If
you see your child
snacking excessively
ask them, "Are
you really hungry or
are you just
unhappy?"
4) Limit
TV watching. For
the average child, watching
television accounts
for 24
hours a week
of sedentary
behavior, and kids frequently eat snacks while watching TV -- not many
calories expended
and
perhaps
even more consumed! A maximum of 2 hours per day of screen time is
recommended.
5) Teach
your child to
"Just Say
No!" to
excess food and junk
food.
Praise him or her
when they resist
temptation.
Post a "No
Pig Out!" sign
on your refrigerator
door (see our No
Pig Out printable poster). Eating
discipline is like
any other form of
discipline, it has
to be taught and
reinforced by the
parents.
6) Your child's
doctor can tell you
if your child is
overweight.
Children and teens less than 19 years of age should not undertake weight loss without the
advice and medical care of a physician.
Children should
not go on severe diets -- their
bodies are growing
and developing,
and they need
adequate nutrition
for maximum height
and good
health. A
better
approach for younger children is to maintain a constant weight or at least slow
their weight gain
until they grow into
their
weight, unless they are severely overweight.
7)
Do
not overly restrict
calories. You
may be encouraging
sneak eating
or binge
eating. Push
better food choices
into the diet and
they will
push out less
desirable
choices. For
example, if veggies
and low-fat
dip are
offered after
school, and cookies
are not easily
available, the
child will
learn to eat what is
offered.
8) Keep
portion sizes
tailored to your
child. Use
smaller plates and
serve
your child
less than you serve
yourself, unless, of
course, your child is
a teen as tall as
you are.
9) All
eating at home needs
to occur at the
kitchen table, even
snacking. No nibbling in
front of the
television, no box
of cookies in the
bedroom,
no
dish of ice cream at
the computer.
10)
Stop offering sweetened beverages, except on special days.
CLICK
HERE FOR ASSOCIATED PRESS WEIGHT MANAGEMENT NEWS
Disclaimer:
The information contained
above should not be used as a substitute
for the medical care and advice of your physician.
There may be variations in treatment that your
physician may recommend based on individual facts
and circumstances.
© 2000 - 2009 eHealth International, Inc.
References:
1. Belluck, P.,
Children's Life
Expectancy Being Cut Short by Obesity, The New York Times, March 17, 2005. (New
England Journal of Medicine article, Dec. 2007)
2. Himes, JH and Deitz, WH. Guidelines for overweight in
adolescent preventive services: recommendations form an expert
committee. American Journal of Clinical Nutrition. 1994;
59:307-316.
3. Pietrobelli, A et al. Body mass index as a measure of adiposity
among children and adolescents: A validation study. Journal of
Pediatrics 1998; 132:204-210.
4. Lazarus, R et al. BMI in screening for adiposity in children and
adolescents: systematic evaluation using receiver operating
curves. American Journal of Clinical Nutrition 1996;63:500-506.
5. Freedman, DS et al. The relation of overweight to
cardiovascular risk factors among children and adolescents: The
Bogalusa Heart Study. Pediatrics 1999;103:1175-1182.
6. Guo, SS et al. The predictive value of childhood BMI values for
overweight at age 35 years. American Journal of Clinical Nutrition
1994:59:810-819.
7. Dietz, WH and Bellizzi, MC. Introduction: the use of BMI to
assess obesity in children. American Journal of Clinical Nutrition
1999;70(suppl):123s-5s.
8. Guo SS and Chumlea, WC. Tracking of BMI in children in
relation to overweight in adulthood. American Journal of Clinical
Nutrition 1999;70(suppl):145s-148s.
9. Barlow, SE and Dietz, WH., Obesity evaluation and treatment:
expert committee recommendations. Journal of Pediatrics 1998;
102(3):e29:
http://pediatrics.aappublications.org/cgi/content/full/102/3/e29
10. Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and
Obesity in Adults, U.S. National Institutes of Health :
http://www.nhlbi.nih.gov/guidelines/obesity/ob_home.htm
11. Rudolf, M., Sahota, P., Barth, J.,
Walker, J., Increasing prevalence of obesity in primary school children: cohort study.,
British Medical Journal, 2001;322:1094-1095 ( 5 May ): http://www.bmj.com/cgi/content/full/322/7294/1094
12. Troiano RP, Flegal KM, Kuczmarski RJ, Campbell SM, Johnson CL, Overweight prevalence and trends for children and
adolescents. The National Health and Nutrition Examination Surveys, 1963 to 1991. Arch Pediatr Adolesc Med. 1995;
149:1085-1091: [Medline
Abstract]
13. Dietz, WH,
and Klish, WJ, Obesity: A Growing Problem, Seminar at the American Academy of
Pediatrics Annual Meeting, San Francisco, October 2001.
14. Belsha, C, and
Blowey, D, New Advances in the Diagnosis and Treatment of Hypertension, Seminar
at the American Academy of Pediatrics Annual Meeting, San Francisco, October
2001.
Back to Top
|
 Because of the current overweight epidemic in
children and teens, for
the first time in history, the current generation of kids is not
expected to live as long as their parents.1
In the United States childhood
obesity has
nearly tripled since 1980 -- 17% of America's
children and
teens are now medically obese, such that their health is
at risk. One out of three is overweight or obese.12 In
Great Britain approximately 16% of children and teens are obese, and the rate is also increasing.11 The problem is worldwide. Overweight children and teens are developing diseases
previously seen only in older adults, such as diabetes (Type 2 ), high blood
pressure, worn-out joints, fatty liver disease, clogged arteries, and sleep apnea
(pauses in breathing). The U.S. Center for Disease
Control now estimates that one in three children born after the year 2000
will develop type 2 diabetes because of the overweight epidemic (see recent
article). The rate will be even higher for African Americans, Hispanics, and Native Americans, where nearly
half of their kids will develop the disease. A new term has been coined, "Diabesity", to
describe the problem. (Diabesity is a registered trademark of
ShapeUp America). Excess weight in the
childhood years can
lead not only to
physical disease but also to psychological
consequences. Overweight children may
develop low self-esteem, limit
activity, and grow to become obese
adults with high risk of diabetes, heart
attacks, strokes, joint failures, and
cancer.
Because of the current overweight epidemic in
children and teens, for
the first time in history, the current generation of kids is not
expected to live as long as their parents.1
In the United States childhood
obesity has
nearly tripled since 1980 -- 17% of America's
children and
teens are now medically obese, such that their health is
at risk. One out of three is overweight or obese.12 In
Great Britain approximately 16% of children and teens are obese, and the rate is also increasing.11 The problem is worldwide. Overweight children and teens are developing diseases
previously seen only in older adults, such as diabetes (Type 2 ), high blood
pressure, worn-out joints, fatty liver disease, clogged arteries, and sleep apnea
(pauses in breathing). The U.S. Center for Disease
Control now estimates that one in three children born after the year 2000
will develop type 2 diabetes because of the overweight epidemic (see recent
article). The rate will be even higher for African Americans, Hispanics, and Native Americans, where nearly
half of their kids will develop the disease. A new term has been coined, "Diabesity", to
describe the problem. (Diabesity is a registered trademark of
ShapeUp America). Excess weight in the
childhood years can
lead not only to
physical disease but also to psychological
consequences. Overweight children may
develop low self-esteem, limit
activity, and grow to become obese
adults with high risk of diabetes, heart
attacks, strokes, joint failures, and
cancer. simply because of the
mechanical stress which the extra weight puts on bone and joint structures.
simply because of the
mechanical stress which the extra weight puts on bone and joint structures.